
Mammograms in Idaho Falls
Common Conditions or Concerns

Treatment Options or Services Provided
A mammogram is a specialized X-ray that captures detailed images of the breast to identify early signs of cancer or other abnormalities—often before they can be felt during a physical exam. Our experienced team ensures every patient feels informed, comfortable, and supported throughout the process.
During your appointment, you can expect:
- A private, professional environment designed for comfort
- Clear communication about what to expect before and during the procedure
- State-of-the-art digital imaging for accurate results
- Review and interpretation by experienced medical professionals
- Coordination with your Family First provider for any necessary follow-up care
We focus on making your screening experience as seamless and reassuring as possible, with prompt results and compassionate guidance every step of the way.
When to Seek Care
You don’t need to wait for symptoms to prioritize your breast health. Consider scheduling a mammogram if you:
- Are age 40 or older and due for your annual screening
- Notice new lumps, changes, or pain in your breasts
- Have a family history of breast cancer or other risk factors
Regular mammograms are one of the most effective tools for early detection—helping identify potential issues when they’re easiest to treat and offering peace of mind through proactive care.
SecondRead AI Technology
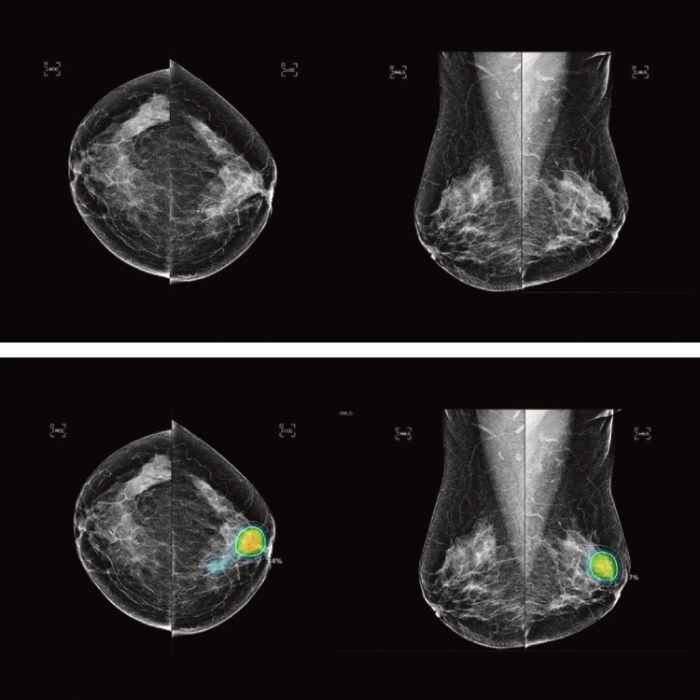
Mammogram FAQ
How do I know if I am at average risk?
The best way to determine if you are at average or high risk for breast cancer is to talk with your health care provider about your family history and your personal medical history. In general, women at high risk for breast cancer include women with a family history of breast cancer in a first degree relative (mother, sister, or daughter), women with an inherited gene mutation, and women with a personal history of breast cancer.
What are the benefits of screening mammography?
Today's high-quality screening mammogram is the most effective tool available to detect breast cancer before lumps can be felt or symptoms appear. Early detection of breast cancer not only helps provide a woman with more choices. It also increases her chances of having the best possible outcome.
What's the difference between a screening mammogram and a diagnostic mammogram?
A screening mammogram is an X-ray of the breast used to detect breast changes in women who have no symptoms, no abnormalities for follow-up, or have 2 years of stable mammograms since their breast cancer diagnosis.
A diagnostic mammogram is for women who have active breast problems or are being followed for a finding on previous breast imaging. Your primary care provider and your radiologist will carefully determine which appointment is best suited for your current needs.
Are mammograms safe?
Mammograms expose the breasts to small amounts of radiation. But the benefits of mammography outweigh any possible harm from radiation exposure. Modern machines use low radiation doses to get breast x-rays that are high in image quality. On average the total dose for a typical mammogram with 2 views of each breast is about 0.4 millisieverts, or mSv. (A mSv is a measure of radiation dose.) The radiation dose from 3D mammograms can range from slightly lower to slightly higher than that from standard 2D mammograms. To put these doses into perspective, people in the US are normally exposed to an average of about 3 mSv of radiation each year just from their natural surroundings. (This is called background radiation.) The dose of radiation used for a screening mammogram of both breasts is about the same amount of radiation a woman would get from her natural surroundings over about 7 weeks. If there’s any chance you might be pregnant, let your health care provider and x-ray technologist know. Although the risk to the fetus is very small, and mammograms are generally thought to be safe during pregnancy, screening mammograms aren’t routinely done in pregnant women who aren't at increased risk for breast cancer.
What should a woman expect when having a mammogram?
Compression may be somewhat painful or uncomfortable. But it is necessary to produce the best pictures using the lowest amount of radiation possible.
Are mammograms painful?
Some women find the pressure of the plates on their breasts to be uncomfortable or even painful. Timing your mammogram when your breasts are not tender is important. In premenopausal women, this is usually 1 week after your menstrual period. If you do experience discomfort or pain, ask the technologist to reposition you to try to make it as painless as possible. Remember that each X-ray takes just a few moments and could save your life.
How do I schedule my appointment?
You can schedule your yearly screening exam without a doctor’s prescription or a screening mammogram order form. Women can self-refer to make an appointment for their annual mammogram for earlier detection of breast cancer.
Breast Cancer Screening Recommendations guidelines for breast cancer screening by
age and risk factor:
age and risk factor:
Beginning at 16 to 18:
Breast cancer is one of the few cancers that can sometimes be felt. It is important to become accustomed to how your breasts naturally feel so that you can recognize any abnormalities. Breast tissue can be lumpy, but if you think you feel something abnormal, you should contact your doctor.
20 onward:
Annual clinical breast exam. This is typically conducted at your yearly gynecological or physical exam.
40 onward:
Annual clinical breast exam and annual mammogram. There is no recommended age at which you should stop receiving annual mammograms, unless you have less than five years of life expectancy due to old age or other illness.
40 onward, with high-risk factors:
Annual clinical breast exam, annual mammogram, breast MRI or breast ultrasound.
How to prepare for your mammogram:
If you’re going to a facility for the first time, bring a list of the places and dates of mammograms, biopsies, or any other breast procedures you’ve had before.
If you’ve had mammograms at another facility, try to get those records to bring with you to the new facility (or have them sent there) so the old pictures can be compared to the new ones.
Schedule your mammogram for when your breasts aren't likely to be tender or swollen, to help reduce discomfort and get good pictures.
On the day of the exam:
Don’t apply deodorant, antiperspirant, powders, lotions, creams, or perfumes under your arms, or on or under your breasts. Some of these contain substances that can show up on the x-ray as white spots. The office will have wipes to help you wipe off deodorant if needed and deodorant wipes for after exam.
You might find it easier to wear a skirt or pants, so that you’ll only need to remove your top and
bra for the mammogram.
Discuss any recent changes or problems in your breasts with your health care provider before
getting the mammogram. (If you have symptoms, you may need a diagnostic mammogram so
special images can be taken of the area of concern.)
Make sure your provider is aware of any part of your medical history that could affect your
breast cancer risk—such as surgery, hormone use, breast cancer in your family, or if you’ve had
breast cancer before.
Don’t be afraid of mammograms!
Remember that only about 2 to 4 screening mammograms in 1,000 lead to a diagnosis of breast cancer.
What to tell your technologist to help ensure you have a good quality mammogram:
Make sure your technologist knows:
About any breast changes or problems, you’re having.
If you have breast implants.
If you have trouble standing and holding still alone (without the aid of a cane or walker).
If you’re breastfeeding or if you think you might be pregnant.
Tell the technologist right away if you start feeling lightheaded or dizzy during the mammogram.
What to expect when getting a screening mammogram:
You’ll have to undress above the waist to get a mammogram. The facility will give you a wrap to wear.
You and the technologist will be the only ones in the room during the mammogram.
To get a high-quality picture, your breast must be flattened or compressed. You'll stand in front of the machine, and the technologist will place your breast on the machine. The plastic upper plate is then lowered to compress your breast for about 10 to 15 seconds while the technologist takes an x-ray. You will then need to change position, so your breast is compressed from side to side before the next x-ray is taken.
If you're getting a 3D mammogram the procedure is the same as above, but you'll notice that the machine will move in a small arc, either over the top of your breast or along the side of your breast, for each image. You might be asked to hold your breath each time it's being done.
The whole procedure takes about 20 minutes. The actual breast compression only lasts about 10 to 15 seconds for each image.
You might feel some discomfort when your breasts are compressed, and for some women it can be painful. Tell the technologist if it hurts so they can try to adjust the compression to your comfort.
Two views of each breast are taken for a screening mammogram. But for some women, such as those with breast implants or larger breasts, more pictures may be needed.
What to expect when getting a diagnostic mammogram:
A diagnostic mammogram is often done if a woman has breast symptoms or if something unusual is seen on a screening mammogram. The basic procedure is similar to that for a screening mammogram, but there are some differences.
More pictures are taken during a diagnostic mammogram, with a focus on the area that looked different on the screening mammogram (or where the symptoms are). These special images may be “spot views” or “magnification views,” which are used to make the area of concern easier to see. Again, if a 3D mammogram is being done, the procedure is the same, but you might be asked to hold your breath while the machine moves in a small arc around your breast to create each image.
What is the difference between a 2D and 3D mammogram?
2D mammograms offer a two-dimensional picture of the breast.
3D mammograms, also known as tomosynthesis, were approved by the FDA in 2011. This newer technology uses multiple low-dose X-ray images from different angles to create a mammogram picture that allows the radiologist to view the tissue in thin "slices."
How will I get my mammogram results?
An approved report of your results will be sent directly to your healthcare provider. You will also receive a letter in the mail with your results within 30 days or as quickly as possible. You may also receive a phone call if the recommendation is for you to receive additional imaging.
Family First FAQ
How do I schedule an appointment?
Call our office directly or send us a message. We offer convenient scheduling options for new and existing patients across all our medical services.
Do you accept insurance?
We work with most major insurance providers. Our billing team can help verify your coverage and explain any out-of-pocket expenses before your visit.
What are your hours?
We are open Monday through Thursday from 7:30am to 6:30pm and Friday from 7:30am to 4:30pm. We offer same-day treatments when possible.
Can I see multiple specialists?
As a comprehensive medical center, we have multiple specialists under one roof. This allows seamless coordination of your healthcare needs across different medical disciplines.
Do you offer telehealth?
Yes, we provide telehealth consultations for certain medical services. Our providers can assess your needs and determine the most appropriate care method.
Testimonials

Everyone who works at Family First Medical is so kind and professional! Whether I’m working with my doctor or nurses, receptionist, or billing, they are knowledgeable.
Morgan


Family First is our family's first choice for our medical care ... health care here has been our family's "go to" provider years.
George
From the moment you walk in, you're greeted by a warm and friendly staff that truly makes you feel at home.
Angie
